
Our hospital emergency departments will administer to around 130,000 patients this year across our Local Health District (LHD) which stretches from Port to Coffs.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
According to LHD data from 2011, our region boasts a population of just over 200,000.
What this means is that six out of every ten people will visit a hospital this year*.
And in the last couple of years, those numbers have been gradually increasing.
While figures would reasonably increase in line with population growth (which sits at around four percent over a six-year period for our region), the real worry is that the increase is largely due to an influx in non-acute patients – that is patients who should probably have gone to see a GP.
We have noticed an increase in our Emergency Department at Macksville, whether that’s related to a shortage of GPs in the community or not, I can’t comment, there might be an association there.
- MNC LHD Chief Executive Stewart Dowrick
“Triage four and five has seen an increase. They are people who come in for what we might call minor ailments, whether it be a cough or a cold etc.
“Our staff have had some peaks but they’ve actually done pretty well to handle it.”
Anecdotally, however, locals have recently had to wait up to nine hours to be seen by a doctor at Macksville Hospital.
And while the impact of Nambucca’s GP shortage is being felt by our hospitals, they are hamstrung in trying to help find a solution to the problem.
The issue? Our hospital systems are governed by the State system, whilst out Primary Health Network (which works closely with GPs) is a Federal beast.
“It is a difficult relationship. State Health is not responsible for the Primary Care space, but we have to work closely with the Primary Health Network and Rural Doctors Network to see whether we can provide better access to general practitioners across our region. And making it sustainable is really important too,” Stewart said.
In order to help those organisations attract GPs to the region, Stewart and his team are planning a number of initiatives including offering administrative and accommodation support services, and advocating to the relevant Federal authority to relabel the Mid North Coast as an ‘area of need’; a classification which attracts increased funding and attention, along with financial incentives for doctors to relocate.
“We can do that and we will do that to advocate for our region,” Stewart said.
“We also have a program that we are starting leading into winter where we’ve identified 500 patients who are regular visitors to the hospital who could be better seen by a primary practitioner. And we’re trying to get GP centres to work with us to treat those people in their practices as opposed to in the hospital.”
Another trial initiative, ‘Integrated Care’, aims to connect selected patients to the Health Direct line where they can receive health advice through a phonecall, in an effort to decongest waiting rooms.
But perhaps the greatest impact the LHD can have on the situation is through the promotion of educational training opportunities for young GPs and specialists.

“With greater opportunities to work or train within regional areas it has been demonstrated that it does make a difference,” Stewart said.
Stewart gives the recent example of the LHD’s involvement in bringing the Australian Indigenous Doctors Association to Bowraville in a visit which aimed to promote a career in health to local Indigenous kids.
READ: Catch up on past EYE ON HEALTH issues
“Shared funding opportunities or flexible funding opportunities between the State and Federal Governments, is also an area that might assist to work through some of these hot spots,” he said.
When asked if Australia might benefit eventually from shifting towards a fully public system of health (as they have in the UK), and have solely one tier of government responsible for it’s management, Stewart was cautiously diplomatic.
“There might be an opportunity for somewhere in Australia to look at a different model, similar to other countries, but you need to study those and work out strengths and weaknesses before you rush into a new system,” he said.
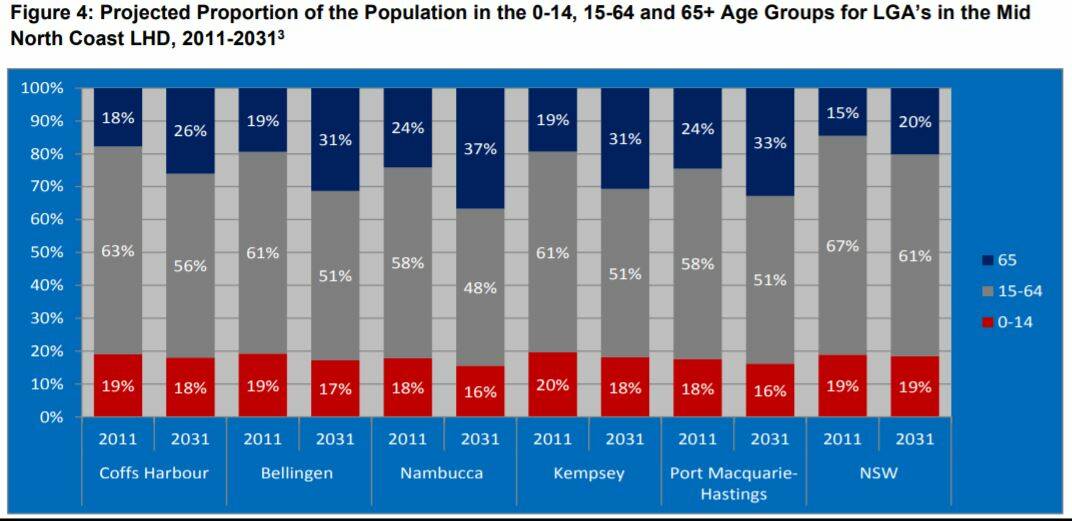
“But these things are always evolving. With an ageing population we may have to reconsider how we deliver health into the future.”
One thing he is confident about is the new infrastructure of the impending Macksville Hospital acting as a beacon for fresh medical talent.
“History suggests that when you build new infrastructure people do alter their decision to come to new communities. It’ll definitely help us attract new medical, nursing and allied health staff to our region,” he said.
But that day is a few years away yet.
- *That proportion is likely to be lower when you take into account people who will use a hospital multiple times throughout the year.


